AS Severity Grading
| Parameter | Mild | Moderate | Severe |
|---|---|---|---|
| Mean gradient (mmHg) | <20 | 20–39 | ≥40 |
| AVA (cm²) | >1.5 | 1.0–1.5 | ≤1.0 |
| Dimensionless index (LVOT VTI / AV VTI) | >0.50 | 0.25–0.50 | <0.25 |
AS Calculator
Severe AVA ≤1.0 cm² or DI <0.25 | Low flow SVI <35 mL/m² | Low gradient <40 mmHg | Reduced EF <50%
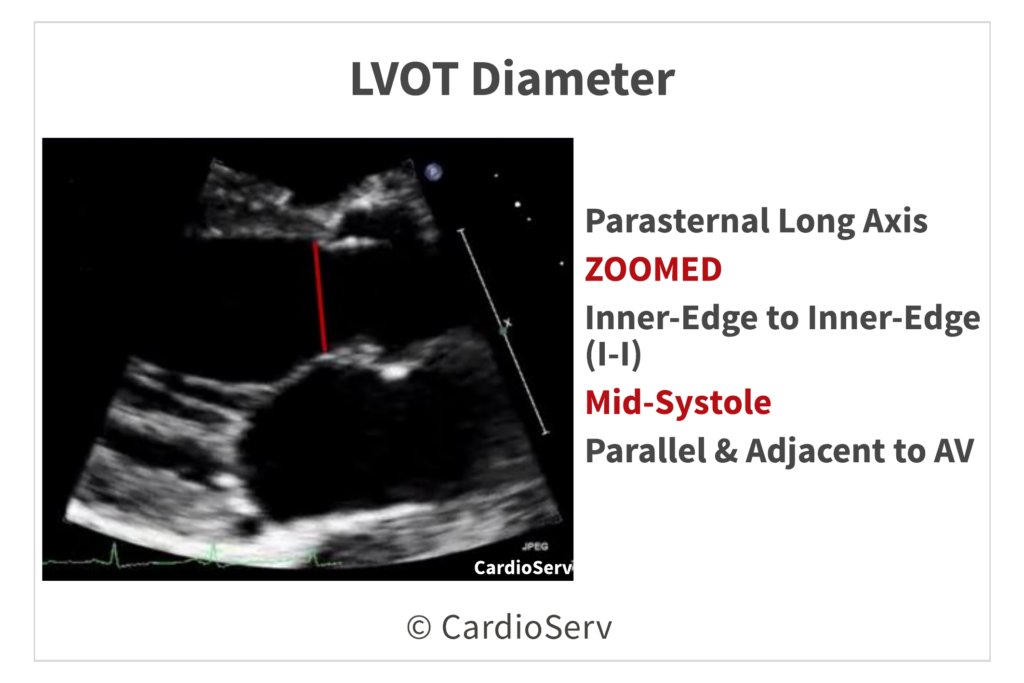
1. LVOT Diameter (PLAX)
- PLAX view
- Zoom on the aortic valve and LVOT
- Timing: Mid-systole (valve open)
- Measure inner-edge to inner-edge
- LVOT Area = 0.785 × (LVOT diameter)²
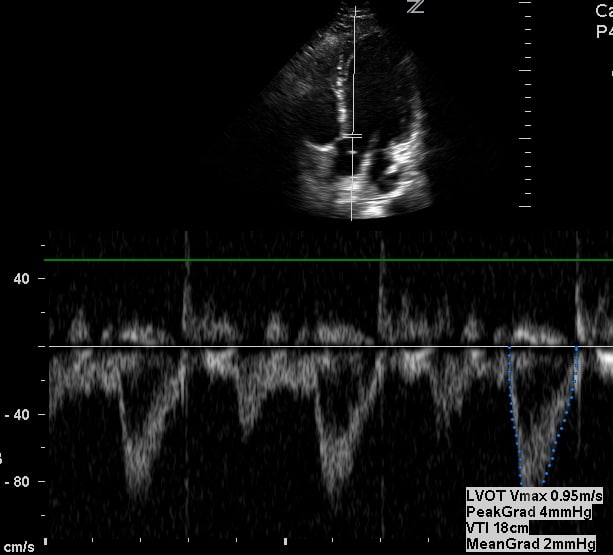
2. LVOT VTI (PW Doppler)
Represents forward stroke flow before the stenotic valve.
- Apical 5-chamber or 3-chamber
- PW doppler
- 0.5–1.0 cm below the aortic valve
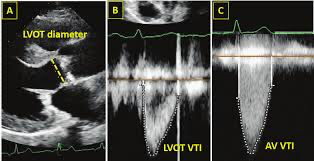
3. Aortic Valve VTI (CW Doppler)
Measures velocity through the stenotic orifice
- CW Doppler
- Use multiple windows:
- Apical 5-chamber
- Apical 3-chamber
- Right parasternal
- Suprasternal notch
- Use the window with the highest reproducible velocity
- Trace the full systolic envelope
- Peak velocity (Vmax)
- Mean gradient
- AV VTI
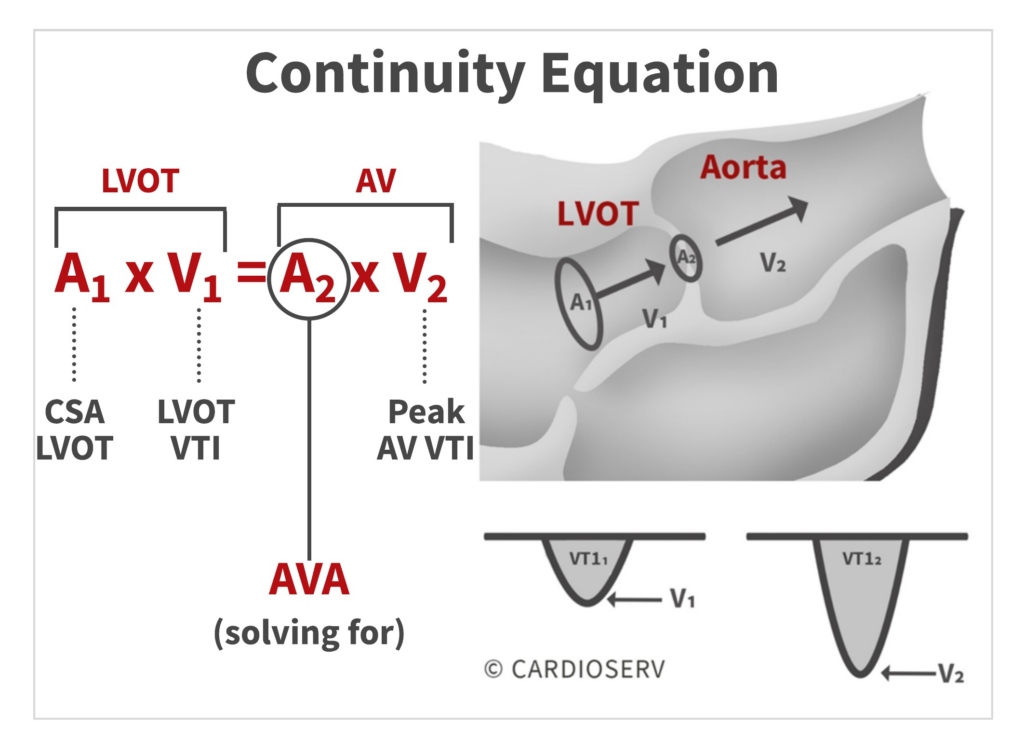
4. Aortic Valve Area (Continuity Equation)
AVA = (LVOT Area × LVOT VTI) ÷ AV VTI
5. Dimensionless Index (DI)
DI = LVOT VTI ÷ AV VTI
- ≤ 0.25 = Severe
- 0.25–0.50 = Moderate
- 0.50 = Mild
6. Gradients
Echo uses the Bernoulli equation:
- ΔP = 4V²
- Peak gradient = highest instantaneous pressure difference
- Mean gradient = average pressure difference across systole
7. Flow State
Stroke Volume = LVOT Area × LVOT VTI
- Index to BSA → SVI
- Low flow if:
- SVI < 35 mL/m²
- Low flow can cause low gradients even if valve is truly severe
